Ovulation Induction
Ovulation induction involves the use of medication to stimulate development of one or more mature follicles (where eggs develop) in the ovaries of women who have an ovulation and infertility. These women do not regularly develop mature follicles without help from ovulation enhancing drugs.
Some of the women with anovulation have a condition known as PCOS or polycystic ovarian syndrome. These women often have irregular menstrual cycles, increased body hair, and infertility.
Who should be treated with induction of ovulation?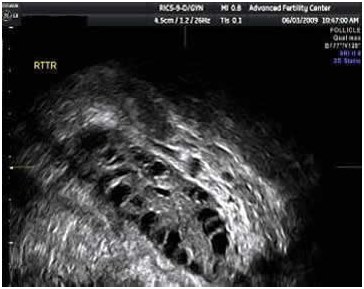
Women, such as those with PCOS, who do not ovulate on their own regularly, and want to get pregnant.
Ultrasound picture of a polycystic ovary from a woman with PCOS – polycystic ovarian diseaseThese women do not develop mature follicles or ovulate without medication treatment About 16 immature follicles (black circular structures) are seen here
Ultrasound photo of a polycystic ovary after Clomid treatment A mature size follicle is now present, as well as some small ones Yellow cursors are on the mature size follicle
Pregnancy success rates for induction of ovulation:
Success rates for induction of ovulation vary considerably and depend on the age of the woman, the type of medication used, whether there are other infertility factors present in the couple, and other factors.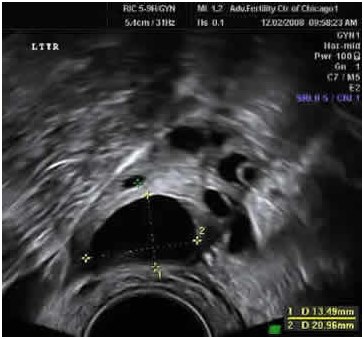
Clomid or Serophene (brand names), clomiphene citrate (generic name) for induction of ovulation
Clomid is an oral tablet that is taken either days 3-7 or 5-9 of the menstrual cycle.
Metformin treatment for women with PCOS, polycystic ovarian syndrome
Metformin (brand name Glucophage) is an oral medication that has been used over the past several years by some infertility physicians to assist in inducing ovulation in some women with anovulation and polycystic ovaries. For more information on metformin therapy, follow the link above.
Fertility drugs after Clomid
Injectable gonadotropins for induction of ovulation
Injectable fertility medications, called gonadotropins, contain follicle stimulating hormone (FSH) which causes development of one or multiple follicles when injected into women that do not ovulate.
These medications are given by intramuscular injections or subcutaneous injections on a daily basis. The injections are started early in the menstrual cycle and are continued for approximately 8-14 days until one or more mature follicles are seen with ultrasound examination of the ovaries. At that point an injection of HCG is given which induces ovulation to occur approximately 36 hours later.
Over 90% of anovulatory women can have ovulation induced with this type of therapy. Pregnancy rates per month are better than those with use of Clomid and for relatively young women with no other contributing causes to the infertility pregnancy rates per month of approximately 15% can be expected when this form of treatment is combined with intrauterine insemination. Pregnancy rates with injectable gonadotropins combined with intercourse are somewhat lower.
This type of therapy is usually tried for 3-6 months and if it does not result in a pregnancy in vitro fertilization should be considered.
Ultrasound and blood monitoring of the stimulation cycle is essential when using injectable gonadotropins as there are substantial risks associated with overstimulation if the ovaries should over respond to the medication.
This monitoring is usually done 3 times a week during the time the woman is taking the injectable medications. This adds substantially to the cost of the cycle. Some health insurance plans will pay for the entire cost of ovulation induction including insemination if that is desired. Other health insurance plans will pay for some (or none) of the costs associated with this treatment.
Complications associated with use of these medications include the possibility of over stimulation, called ovarian hyper stimulation syndrome, or OHSS. OHSS is reported to occur in approximately 1% of cycles. Hyper stimulation involves enlarged ovaries, abdominal pain, and fluid build-up within the abdomen. It may require hospitalization in extreme cases to control pain or manage the syndrome. Carefully monitored use of inject able gonadotropins can almost always avoid severe over stimulation.
Multiple pregnancy is also a possibility when these medications are used. In general approximately 75% are single, 20% are twins, 5% are triplets and 1% are quadruplets or higher.
When many mature follicles develop the couple and the physician can have a discussion about the risks of multiple pregnancy and there is always the option of canceling the cycle by not giving the injection that causes ovulation. This essentially eliminates the risk of any pregnancy (single or multiple) occurring in that cycle.
Bromocriptine for induction of ovulation
Anovulation caused by elevated levels of the piuitary hormone hormone prolactin can be treated with a medication called bromocriptine. This is an uncommon anovulation disorder. Women with this condition often have no menstrual periods – amenorrhea.
Intra- Uterine Insemination
What is IUI? Intrauterine insemination is also called IUI or artificial insemination.
- Insemination of domestic and farm animals has been done since the early 1900′
- Human artificial insemination with the male partner’s sperm forinfertility began being used in the 1940’s
The IUI procedure can be an effective treatment for some causes of infertility
IUI is commonly used for unexplained infertility. It is also used for couples affected by mild endometriosis, problems with ovulation, mild male factor infertility and cervical factor infertility.
Insemination is a reasonable initial treatment that should be utilized for a maximum of about 3 months in women who are ovulating (releasing eggs) on their own. It is reasonable to try IUI for longer in women with polycystic ovaries (PCOS) and lack of ovulation that have been given drugs to ovulate.
Artificial insemination should not be used in women with blocked fallopian tubes. The tubes are often checked out with an x-ray test called a hysterosalpingogram.
Female age is a significant factor with IUI. Intrauterine insemination has very little chance of working in women over 40 years old. IUI has also been shown to have a reduced success rate in younger women with a significantly elevated day 3 FSH level, or other indications of significantly reduced ovarian reserve.
If the sperm count, motility and morphology scores are quite low, intrauterine insemination is unlikely to work.
- With significant male factor issues,IVF with ICSI is indicated and has high success rates
How is insemination performed? What is the process for artificial insemination in humans?
- The woman usually isgiven medications to stimulate development of multiple eggs and insemination is timed to coincide with ovulation – release of the eggs.
- A semen specimen is either produced at home or in the office by masturbation after 2-5 days of abstinence from ejaculation.
- The semen is “washed” in the laboratory (called sperm processing or sperm washing). The sperm is separated from the other components of the semen and concentrated in a small volume. Various media and techniques can be used for the washing and separation. Sperm processing takes about 30-60 minutes.
- A speculum is placed in the vagina and the cervical area is gently cleaned.
- The washed specimen of highly motile sperm is placed either in the cervix (intracervical insemination, ICI) or higher in the uterine cavity (intrauterine insemination, IUI) using a sterile, flexible catheter.
The intrauterine insemination procedure, if done properly, should seem similar to a pap smear for the woman. There should be little or no discomfort.
Most clinics offer for the woman to remain lying down for a few minutes after the procedure, although it has not been shown to improve success. The sperm has been put above the vagina and cervix – it will not leak out when you stand up.
- Assisted Reproductive Techniques- IVF,ICSI
What is in vitro fertilization – IVF?
The IVF process involves:
- Stimulating multiple folliclesand eggs to develop
- Egg retrievalto get the eggs
- Fertilizing the eggs in thelaboratory
- Embryo transferto the uterus
- Louise Brown was the first IVF baby in the world. She was born in July of 1978 in England.
- Louise was 28 (in 2006) when she had her own baby (not IVF)
- Hundreds of thousands of children are born every year after IVF treatments
- Well over 5 million babies have been born with IVF
Who should be treated with in vitro fertilization?
IVF can be used as an effective treatment for infertility of all causes except for women with infertility caused by an anatomic problem with the uterus, such as severe intrauterine adhesions.
It is generally used in couples who have failed to conceive after at least one year of trying who also have one or more of the following:
- Blocked fallopian tubes or pelvic adhesionswith distorted pelvic anatomy. Women that have had tubal ligation and are considering tubal reversal surgery as well as men that are considering vasectomy reversal surgery might also consider IVF.
- Male factor infertility(low sperm count or low motility). ICSI is an IVF procedure that can fertilize eggs even with poor sperm quality.
- Failed 2-4 cycles ofovarian stimulation with intrauterine insemination
- Advanced female age – over about 38 years of age.
- Reduced ovarian reserve, which means lower quantity (and sometimes quantity) of eggs. Aday 3 FSH and estradiol test, antral follicle counts and AMH hormone levels are often done as screening tests for egg quantity. Reduced egg quantity and quality is usually treated with either IVF, or with IVF with egg donation.
- Severeendometriosis
- Unexplained infertilitywhen inseminations have failed. Unexplained infertility means standard fertility tests have not found the cause of the fertility issue.
How does IVF improve fertility?
In vitro fertilization increases the efficiency of human reproduction, which is often not very efficient naturally.
- Essentially, it is a numbers game that worsens as the female partner ages
- With IVF we remove multiple eggs – and after careful culture for 3-5 days of the eggs that fertilize, we transfer one or more of the “prettiest” embryos back to the uterus.
- Any remaining embryos (if there are any) can be frozen for future use by the couple
In a sense, we compress many months of “natural” attempts into one menstrual cycle. By transferring the fertilized embryo(s) directly to the uterine cavity, fertility is improved for many couples that have sperm issues (fertilization defects), or issues on the female side related to egg pickup from the ovary, or tubal transport of the embryo to the uterus.
Therefore, with IVF:
- We stimulate with medications to produce multiple follicles and eggs (only one follicle with one egg inside develops in a natural menstrual cycle)
- We retrieve the eggs from the ovaries when they’re ready (release and tubal pickup of the egg can be inefficient naturally)
- We coercefertilization in the lab (sperm or egg issues can cause fertilization problems in a natural situation)
- We culture the embryos for several days and then pick the best one (or more) for transfer to the woman – selection of the best one(s) increases success.
- We transfer the embryos to the best location in the middle of the uterine cavity (tubal transport of the embryo to the uterus is bypassed)
- Fertility Preservation (Egg and Sperm freezing)
What is egg freezing and why do it?
Egg freezing is a relatively new technique that allows mature eggs to be stored for a long time at very low temperatures. The eggs are cryopreserved using the ‘vitrification’ method (also known as fast freezing) before they are stored in liquid nitrogen at -196°C until they are going to be used. The eggs can then be stored for up to 10 years. In some cases the storage period can be extended beyond 10 years, but this is not true for everyone.
Egg freezing is used for both social and medical reasons. Many women are now waiting until later life before trying to have a baby, this however presents a number of challenges. Egg freezing can overcome some of these challenges by giving women the opportunity to retrieve and store their eggs whilst they are younger, during their prime reproductive years. The eggs can then be used later in life during a cycle of ICSI treatment to help achieve a pregnancy. Other women may decide to freeze their eggs for medical reasons.These women may have experienced premature ovarian failure, undergone surgery to remove their ovaries or needed chemotherapy or radiotherapy to treat cancer. All of these things will affect your fertility, meaning that egg freezing could help you in the future to achieve a pregnancy.
What is involved in freezing my eggs?
To maximise the chances of freezing eggs successfully, the ovaries are stimulated using daily fertility drugs. This encourages them to produce more than one follicle during the stimulated cycle. The egg itself is growing within the follicle. Pelvic ultrasound monitoring is used to check the ovaries and to see how many follicles might be developing. Blood tests may also be needed to check the hormone levels in the body.
When at least 3 follicles measuring more than 17mm in diameter are seen, a hormone injection is given to ripen and mature the eggs. Egg collection is then carried out under sedation approximately 36 hours later. This procedure takes about 20 minutes and involves removing the fluid from each follicle. The embryologists then examine the fluid under the microscope to see if an egg is present. Eggs are then checked to see if they are mature or not. Not every egg is mature when they are collected. All mature eggs are ready to receive a sperm cell and are cryopreserved using the fast freeze or vitrification method.
What happens when I want to use my eggs?
When you decide you want to use your eggs you will need to undergo an ICSI treatment cycle. Find out more about ICSI. At the appropriate time the eggs will be thawed and it is important to note that not all eggs will survive the thawing process. These eggs are then fertilised by injecting the sperm into the egg.
What are the outcomes using frozen eggs?
As egg freezing is relatively new there is a not a huge amount of data on risks and success rates. Research has not shown any link between using a frozen egg for treatment and giving birth to a baby with a birth defect or chromosomal abnormalities. The chance of having a live birth using a frozen egg is currently around 15%.
Why is sperm frozen?
Sperm is often frozen for medical reasons. Some forms of chemotherapy, radiotherapy and surgery can affect fertility on a temporary or permanent basis. Before any of these procedures are carried out, it is possible to store sperm using a freezing method called cryopreservation. Sperm is also frozen if healthy samples are retrieved following Surgical Sperm Retrieval.
What happens when the sperm is needed?
At the appropriate time the samples are thawed and checked. It is important to note that not all sperm will survive the thawing process. Healthy sperm from the samples are then used for fertility treatments such as IVF, ICSI and IUI.
What are the success rates for using frozen sperm?
Sperm freezing has been used successfully for many years but the success of the treatment comes down to the quality of the sperm stored. Poor sperm samples which have been frozen are less likely to be successful than healthy sperm samples, or may only be successful with more invasive types of treatments such as ICSI.
- Donor treatment
Who should be treated with IVF using donor eggs?
Egg donation (oocyte donation or ovum donation) is an effective treatment for infertility except in women with a severe uterine problem, such as extensive intrauterine adhesions.
Success rates with egg donation are high, particularly compared to pregnancy rates in women with poor egg quality and quantity.
Donor egg IVF is generally used in women with significantly diminished egg quantity and quality (poor ovarian reserve). This includes women with:
- Premature ovarian failure (early menopause)
- Very poor egg quality
- Poor response to ovarian stimulation
- Highday 3 follicle stimulating hormone (FSH) levels
- Very lowantral follicle counts on ultrasound
Advanced female age, such as over age 40





 WhatsApp us
WhatsApp us